AI model detects hidden pancreatic cancer up to 3 years before doctors spot it on CT scans
3 Sources
[1]
New AI model spots hidden pancreatic cancer long before diagnosis
By Dr. Sanchari Sinha Dutta, Ph.D.Reviewed by Lauren HardakerMay 7 2026 A next-generation AI model uncovers invisible signs of pancreatic cancer on standard CT scans long before symptoms appear, potentially transforming early detection and improving outcomes in one of the deadliest cancers Study: Next-generation AI for visually occult pancreatic cancer detection in a low-prevalence setting with longitudinal stability and multi-institutional generalisability. Image credit: crystal light/Shutterstock.com Mayo Clinic researchers have developed an artificial intelligence-powered model that can detect pancreatic cancer on routine abdominal CT scans well before its clinical diagnosis. The study is published online in the journal Gut. Why pancreatic cancer is usually detected too late Pancreatic cancer is one of the deadliest cancers with a five-year survival rate of less than 15 %. It has been predicted to be the second leading cause of cancer-related deaths in the United States by 2030. The diagnosis of pancreatic cancer is primarily based on its symptoms, which mostly remain undetectable at early stages. Because of this reason, more than 85 % of cases remain undiagnosed until the cancer spread to other organs and become unmanageable by therapeutic interventions. Early detection is considered the most effective strategy to improve overall survival of pancreatic cancer. Glycemically-defined new onset diabetes (gNOD) is gaining interest as an early clinical sign of pancreatic cancer, and the National Institute for Health and Care Excellence (NICE) currently recommends urgent abdominal CT scans for individuals aged 60 years or older with gNOD and weight loss. However, conventional imaging often fails to detect malignant lesions at a curable stage due to certain factors, including perceptual error, technical problems, or absence of any discernible mass (imaging-occult). To overcome these limitations and improve early diagnosis, researchers at Mayo Clinic, USA, developed a new-generation AI model named Radiomics-based Early Detection Model (REDMOD) to identify apparently invisible subclinical alterations of pancreatic cancer at a pre-clinical (stage 0) phase that may be amenable to curative intervention. The researchers trained their AI model with 156 pre-diagnostic and 813 control abdominal CT scans (controls confirmed to have no evidence of pancreatic ductal adenocarcinoma, with benign findings permitted) from multiple institutes. Pre-diagnostic scans referred to incidental CTs obtained months to years prior to clinical diagnosis of pancreatic cancer. The model was subsequently validated using an independent set of abdominal CT scans, including 63 pre-diagnostic and 430 control scans. AI detects hidden pancreatic cancer months before diagnosis The validation analysis using the independent test set revealed that the AI model REDMOD can identify 73 % of those pre-diagnostic cancers at a median lead time of approximately 16 months before clinical diagnosis, achieving an area under the curve (AUC) of 0.82. This corresponded to nearly 2-fold higher detection rate than specialists reviewing the same scans without AI assistance. The detection rate increased to nearly 3-fold for scans obtained more than two years before diagnosis. Notably, the AI model exhibited consistent and stable predictive accuracy over time across CT scans obtained from multiple institutions, imaging systems, and protocols. Furthermore, the model consistently predicted the same results in patients with multiple scans obtained months apart. These features support its clinical use for early detection and longitudinal monitoring. The mechanistic analysis showed that the model can capture even subtle biological changes at the early stage of cancer development by analyzing several quantitative imaging features that describe tissue texture and structure. The exclusive inclusion of filtered radiomic features was found to be the primary drivers of the predictive ability of the model. Early AI detection could enable intervention before symptoms The study describes the development and validation of a fully automatic AI model that outperformed radiologists in terms of identifying apparently invisible clinical signs of pancreatic cancer on routine abdominal CT scans that were obtained for other reasons up to three years before the clinical cancer diagnosis. This early detection of pancreatic cancer well before the appearance of visible tumor mass could have significant clinical implications by enabling earlier intervention, potentially improving cancer prognosis. The detection of pancreatic cancer at a potentially curable pre-clinical stage would be particularly vital for high-risk individuals, including those with gNOD and weight loss. Overall, the study findings highlight the significance of implementing AI-powered workflow in clinical settings to improve the accuracy of early cancer detection. However, the model achieved a specificity of about 81 % and a relatively modest precision, highlighitng the importance of managing false positives in screening contexts. In absence of visible cancerous changes, there remains a risk of automation bias where readers uncritically accept AI predictions. To address automation bias, researchers are advancing their work using Artificial Intelligence for Pancreatic Cancer Early Detection, or AI-PACED, an upcoming prospective study that will quantify automation bias and establish optimal override criteria so that algorithmic alerts prompt appropriate risk-stratified evaluation rather than premature intervention. They are also combining AI analysis of routine imaging with longitudinal follow-up to assess performance, including early detection, false positives, and clinical outcomes. With further clinical validations, the AI model REDMOD could serve as a triage and longitudinal monitoring tool to overcome the negative consequences of deadliest pancreatic cancer associated with late-stage symptomatic diagnosis. The study did not validate the performance of REDMOD across different racial and ethnic groups. Future studies should focus on this matter given known disparities in pancreatic cancer risk among individuals with gNOD. Download your PDF copy by clicking here. Journal reference: Mukherjee S. (2026). Next-generation AI for visually occult pancreatic cancer detection in a low-prevalence setting with longitudinal stability and multi-institutional generalizability. Gut. DOI: https://gut.bmj.com/content/early/2026/04/22/gutjnl-2025-337266. https://gut.bmj.com/content/early/2026/04/22/gutjnl-2025-337266
[2]
New AI model spots pancreatic cancer up to 3 years earlier than human doctors in test
A new AI tool finds early hints of pancreatic cancer in CT scans that doctors would otherwise miss, an early test found. A new artificial intelligence (AI) model can help doctors detect pancreatic cancer up to three years before physicians typically spot tumors on CT scans, a new study suggests. The program, described April 28 in the journal Gut, was used to analyze almost 2,000 CT scans that had been previously cleared as "normal," bearing no signs of disease. The tool identified tiny irregularities in the structure of the pancreas that later developed into tumor tissue. Early detection is the single biggest factor in pancreatic cancer patients' survival. Therefore, the model could potentially enable physicians to begin effective treatment while the disease is still curable, the study authors said. A chance to detect cancer early Pancreatic cancer is one of the deadliest cancers. "The five-year survival rate [in the U.S.] is about 12% to 13% because of our inability to detect it at a time when therapeutic options could work their magic," study co-author Dr. Ajit Goenka, a radiologist and nuclear medicine specialist at the Mayo Clinic in Rochester, Minnesota, told Live Science. The early stages of pancreatic cancer often don't trigger any symptoms, so the disease is often advanced at the point of diagnosis. Although doctors' ability to catch and treat many other cancers has improved in recent decades, no corresponding breakthrough has been seen in pancreatic cancer. Diagnosis typically involves a combination of tissue sampling and imaging tests, including CT scans. But by the time tumors are visible via these methods, the cancer is often terminal. However, there may be earlier markers of the disease. "The basic science research tells us that the process of cancer development is not something that starts six months earlier," Goenka said. "It starts 10 to 15 years earlier, which means that there was a signal in the pancreas and that signal was outside the purview of human detectability." Leveraging AI to recognize patterns that humans cannot, Goenka and colleagues developed a tool to amplify that existing signal and identify early signs of disease in CT scans. The model, dubbed Radiomics-based Early Detection Model (REDMOD), essentially converts the CT scan image into a mathematical puzzle. It first segments the organ, building a 3D model of the pancreas from the 2D images captured by the CT machine. Then, it evaluates the resulting structure pixel by pixel. "It's taking each and every pixel in that image and it is quantifying the degree to which it differs from the rest of the organ, and then it's comparing that against the controls where you don't expect that change to be present," Goenka explained. "At the end of the day, it's mathematics. It converts that image into a mathematical representation and extracts those mathematical features." The team tested the model on a sample of 2,000 existing CT scans, which were previously collected for medical issues unrelated to cancer and had all been signed off as normal. About one-seventh of the scans belonged to patients who later went on to develop pancreatic cancer. The model successfully identified 73% of these early-stage cases, and on average, the scans the model analyzed had been taken 16 months before the person's actual diagnosis. "The sensitivity gain over radiologists was nearly twofold across the spectrum, and when you look at even earlier -- more than two years prior to diagnosis -- that sensitivity gain was almost threefold," Goenka said. In other words, the AI tool correctly identified cancer cases earlier than radiologists did, and the earlier in time you look, the greater that performance gap grew. Next steps That said, the AI tool has room for improvement. "The radiologist was less likely to flag a healthy patient incorrectly," Goenka noted. The model correctly identified disease-free patients 81.1% of the time, compared with an average of 92.2% for human radiologists. "So there is a complementary role for both of them, for physician expertise combined with AI augmentation." The study was very well designed and produced some extremely promising results, said Tatjana Crnogorac-Jurcevic, a professor of molecular pathology and biomarkers at Queen Mary University of London who was not involved in the work. "Such early detection would make a huge change in the clinical workup of the patients," she told Live Science. "Because pancreatic cancer is fairly uncommon, general screening as we have now for colon and breast is not going to be feasible, but there are defined high-risk groups for which surveillance will be possible -- individuals with a family history of pancreatic cancer, those with other cancer mutations, and patients with new-onset diabetes." Goenka hopes the model could be routinely implemented in the clinic within the next five years, and the team is currently running clinical trials to further validate that this detection strategy works in practice. Looking forward, combining this REDMOD with other diagnostic methods could yield even greater gains in early detection, Crnogorac-Jurcevic said. "We are developing urine-based tests with exactly the same aim, and having an AI imaging tool to combine with our body fluid biomarkers would be fantastic," she said. "It's highly likely that they will be complementary, which would increase the sensitivity and accuracy of early detection massively."
[3]
AI learned to spot invisible signs of deadly pancreatic cancer before diagnosis
A new artificial intelligence system has detected early traces of pancreatic cancer in normal-looking scans an average of 475 days before patients were diagnosed. That extra time could move some patients toward surgery before the disease spreads beyond reach. Inside routine abdominal CT scans, the pancreas looked normal to specialists. By tracking patterns too faint for the eye, Ajit Harishkumar Goenka, M.D., at Mayo Clinic connected those clean-looking images to cancers diagnosed months or years later. Goenka's team tested the Radiomics-based Early Detection MODel (REDMOD) on 1,462 scans, including 219 from people whose earlier images looked cancer-free before diagnosis. That gap between a clean-looking scan and a later diagnosis is the clinical opening the system could turn into usable time. Pancreatic ductal adenocarcinoma, the common form that starts in duct-lining cells, kills so often because doctors usually meet it late. By the time pain, weight loss, jaundice, or digestive trouble pushes someone into testing, the tumor has often spread beyond surgery. The National Cancer Institute (NCI) estimates 67,530 new U.S. cases and 52,740 deaths in 2026, with far better survival when cancer remains confined to the pancreas. "Modeling studies show that increasing the rate of localized pancreatic carcinomas from 10% to 50% could more than double survival rates," wrote Goenka and colleagues. The system does not look for a hidden lump. Instead, it measures computer-counted patterns in tissue texture across the whole pancreas, where early cancer may disturb the organ before forming a mass. Many useful signals came from digital filters that sharpened fine texture differences, which means the model drew power from structure rather than a doctor-style visual clue. That mechanism matters because an alert based on shape alone would fail when the organ still looks normal. Two abdominal radiologists reviewed the same independent test set without knowing which scans later belonged to cancer patients. The AI identified 73% of pre-diagnostic cases, while the doctors found about 39%. On scans taken more than two years before diagnosis, the gap widened: 68% for the system and 23% for the radiologists. Those results do not make doctors obsolete; they show that the earliest signal was not one human eyesight was built to catch. High sensitivity, which means catching true cases, came with trade-offs. In the independent test set, REDMOD correctly cleared about 81% of people without pancreatic cancer, which leaves room for false alarms. A false alarm can send a patient into extra imaging, worry, and sometimes invasive testing, so a future clinical tool would need a careful follow-up plan. Screening earns trust only when it finds dangerous disease early without flooding clinics with low-risk scares. Broad screening for everyone would make little sense because pancreatic cancer remains rare. Doctors would probably start with people whose risk is already higher, such as older adults with unexplained weight loss or new diabetes. In the United Kingdom, the National Institute for Health and Care Excellence (NICE) already advises urgent CT or ultrasound for people 60 and older with weight loss plus new-onset diabetes. An AI flag could make that kind of pathway sharper, but only if testing proves it improves outcomes rather than just labels risk earlier. Early-warning software cannot help much if it gives different answers every time a person is scanned. REDMOD's predictions agreed on repeat scans in 90% to 92% of cases, a sign that the signal was not random noise. In some patients, the same risk pattern appeared months apart before doctors could see a tumor. That steadiness supports monitoring over time, where a single alert might trigger closer watching instead of immediate intervention. Looking back at old scans can point the way, but it cannot prove that patients will live longer when doctors use the system. Future trials must test real patients before diagnosis, measure false positives, and track whether earlier alarms actually lead to curative treatment. The dataset also needs deeper checks across race, ethnicity, scanners, hospitals, and image quality. Without that work, an impressive model could still miss people or overburden clinics outside the research setting. Clinical value depends on what happens after a warning. Someone with a high-risk result might receive repeat imaging, blood tests, or endoscopic ultrasound. Surgery would still require proof of disease, because removing pancreatic tissue can carry serious risks. Used carefully, the system could become a triage tool rather than a stand-alone diagnosis. The finding reframes a normal-looking pancreas as a possible source of early warning, not because doctors missed a visible tumor, but because software found texture changes beneath ordinary vision. Real benefit will depend on prospective trials, clear thresholds, and careful follow-up that protects patients from both late diagnosis and needless alarm. Like what you read? Subscribe to our newsletter for engaging articles, exclusive content, and the latest updates.
Share
Copy Link
Mayo Clinic researchers developed REDMOD, an AI model that identifies pancreatic cancer on routine CT scans an average of 16 months before clinical diagnosis. The system detected 73% of pre-diagnostic cases that appeared normal to radiologists, with detection rates nearly three times higher for scans taken more than two years before diagnosis. This breakthrough could enable earlier intervention in one of the deadliest cancers.
AI Model Outperforms Radiologists in Spotting Invisible Cancer Signs
Researchers at Mayo Clinic have developed an AI model called Radiomics-based Early Detection Model (REDMOD) that can detect early signs of pancreatic cancer on routine abdominal CT scans well before symptoms emerge
1
. Published in the Gut journal, the study demonstrates how AI for cancer detection is transforming the landscape of pre-diagnostic detection for one of medicine's deadliest malignancies2
.
Source: Earth.com
The system identified 73% of hidden pancreatic cancer cases at a median lead time of approximately 16 months before clinical diagnosis, achieving an area under the curve (AUC) of 0.82
1
. This represents nearly a twofold higher detection rate than specialists reviewing the same scans without AI assistance. For scans obtained more than two years before diagnosis, the detection rate increased to nearly threefold, with the AI identifying 68% of cases compared to just 23% for radiologists3
.Why Early Detection Matters for Pancreatic Cancer Survival
Pancreatic cancer remains one of the deadliest cancers, with a five-year survival rate of less than 15% in the United States
1
. According to Ajit Goenka, study co-author and radiologist at Mayo Clinic, "The five-year survival rate is about 12% to 13% because of our inability to detect it at a time when therapeutic options could work their magic"2
. The disease has been predicted to become the second leading cause of cancer-related deaths in the United States by 20301
.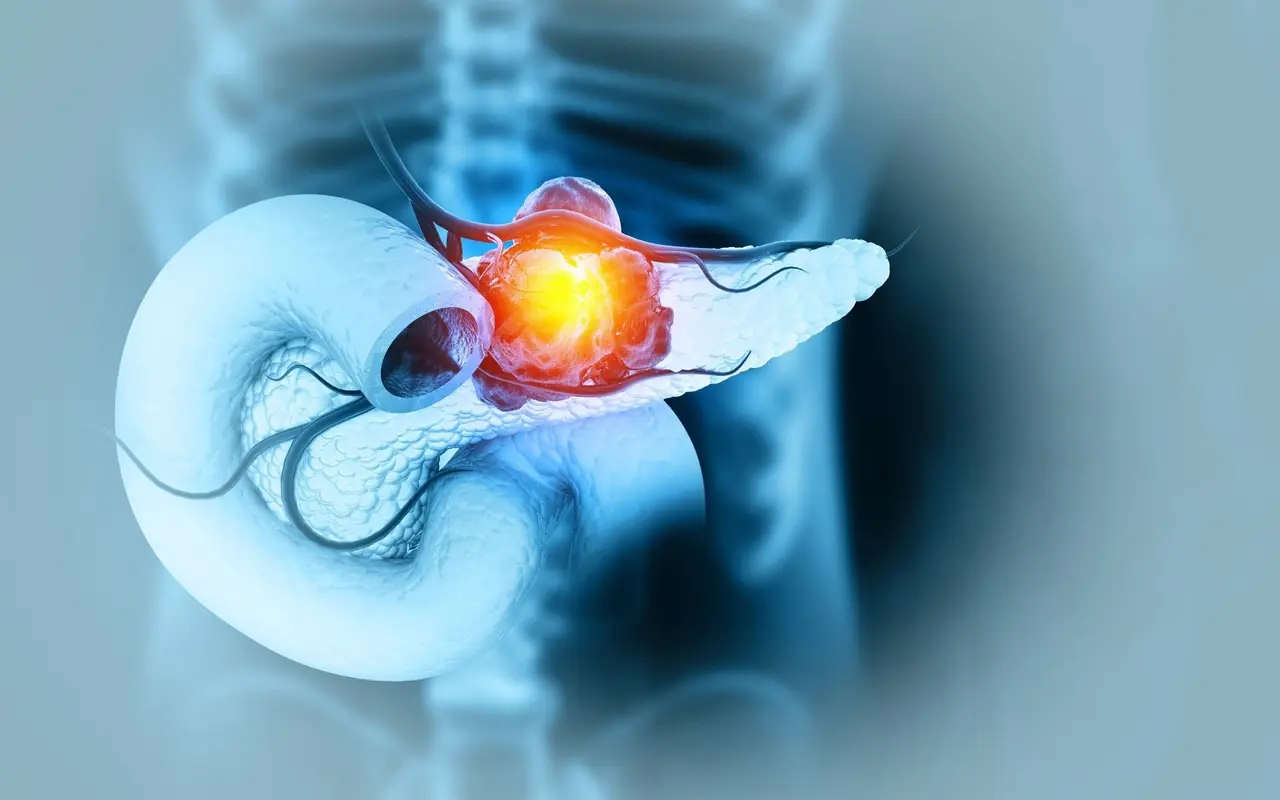
Source: News-Medical
More than 85% of pancreatic cancer cases remain undiagnosed until the cancer spreads to other organs and becomes unmanageable by therapeutic interventions
1
. The National Cancer Institute estimates 67,530 new U.S. cases and 52,740 deaths in 2026, with survival rates dramatically better when cancer remains confined to the pancreas3
. Modeling studies show that increasing the rate of localized pancreatic adenocarcinoma detection from 10% to 50% could more than double survival rates3
.How REDMOD Detects Cancer on CT Scans Using Radiomics
The researchers trained REDMOD with 156 pre-diagnostic and 813 control abdominal CT scans from multiple institutes, then validated it using an independent set including 63 pre-diagnostic and 430 control scans
1
. The system converts CT scan images into mathematical representations, building a 3D model of the pancreas from 2D images and evaluating tissue texture pixel by pixel2
."It's taking each and every pixel in that image and it is quantifying the degree to which it differs from the rest of the organ, and then it's comparing that against the controls where you don't expect that change to be present," Goenka explained
2
. The mechanistic analysis revealed that the model captures subtle biological changes by analyzing quantitative imaging features that describe tissue texture and structure, with filtered radiomic features serving as primary drivers of predictive ability1
.Balancing Sensitivity and Specificity in AI-Powered Workflows
While REDMOD demonstrates superior sensitivity in improving survival rates through early detection, it achieved a specificity of about 81.1% in correctly identifying disease-free patients, compared with an average of 92.2% for human radiologists
2
. This false positive rate means some healthy patients could face additional imaging, worry, and potentially invasive testing3
."The radiologist was less likely to flag a healthy patient incorrectly," Goenka noted. "So there is a complementary role for both of them, for physician expertise combined with AI augmentation"
2
. The system exhibited consistent and stable predictive accuracy over time, with predictions agreeing on repeat scans in 90% to 92% of cases, supporting its use as a triage tool for longitudinal monitoring1
3
.Related Stories
Targeting High-Risk Groups for Maximum Impact
Broad screening for everyone would make little sense because pancreatic cancer remains relatively rare
3
. According to Tatjana Crnogorac-Jurcevic, professor of molecular pathology at Queen Mary University of London, "There are defined high-risk groups for which surveillance will be possible—individuals with a family history of pancreatic cancer, those with other cancer mutations, and patients with new-onset diabetes"2
.The National Institute for Health and Care Excellence (NICE) currently recommends urgent abdominal CT scans for individuals aged 60 years or older with glycemically-defined new onset diabetes and weight loss
1
. An AI flag could sharpen these clinical pathways, though testing must prove it improves outcomes rather than simply labeling risk earlier3
.What Comes Next for Clinical Trials and Implementation
Goenka hopes the model could be routinely implemented in clinics within the next five years, with clinical trials currently underway to further validate pre-diagnostic detection capabilities
2
. Future trials must test real patients before diagnosis, measure false positives, and track whether earlier alarms actually lead to curative treatment3
.The dataset also requires deeper validation across race, ethnicity, scanners, hospitals, and image quality to ensure the augmented intelligence system performs reliably outside research settings
3
. Someone with a high-risk result might receive repeat imaging, blood tests, or endoscopic ultrasound, though surgery would still require proof of disease given the serious risks of removing pancreatic tissue3
. The system's ability to detect cancer on CT scans obtained for unrelated medical issues positions it as a potentially valuable screening layer within existing abdominal imaging workflows.References
Summarized by
Navi
[2]
Related Stories
AI detects pancreatic cancer up to 3 years before diagnosis, outperforming radiologists by nearly 3x
29 Apr 2026•Health

AI Breakthrough: Deep Learning Model Revolutionizes Pancreatic Cancer Diagnosis and Treatment
13 Dec 2024•Health

ChatGPT-4 Matches Radiologists in Pancreatic Cyst Analysis, Promising Efficient Healthcare
16 Jul 2025•Health

Recent Highlights
1
Anthropic overtakes OpenAI as most valuable AI startup with $965 billion valuation
Business and Economy

2
Apple's Siri overhaul for iOS 27 brings Gemini integration and standalone app to compete with ChatGPT
Technology

3
Pope Leo XIV releases major AI encyclical calling for 'disarmament' of artificial intelligence
Policy and Regulation





