AI detects pancreatic cancer up to 3 years before diagnosis, outperforming radiologists by nearly 3x
9 Sources
[1]
AI Spots Pancreatic Cancer Years Before It Shows Up, Study Finds
The system could eventually be used to flag high-risk patients for closer follow-up, but it needs prospective testing to confirm it improves outcomes before routine use. An artificial intelligence system can spot pancreatic cancer long before it shows up on scans, raising the prospect of catching one of the deadliest tumors early enough to successfully treat, a study found. The model, developed by researchers at the Mayo Clinic and collaborators, identified subtle changes in routine CT scans an average of about 475 days before patients were diagnosed, according to the study, published Tuesday in the journal Gut. Pancreatic cancer is rarely detected early because tumors typically don't cause symptoms and often aren't visible on imaging until the disease is advanced. More than 85% of cases are found at a stage where treatment is largely limited to easing symptoms, helping explain why five-year survival is about 10% globally. The findings point to a potential shift in how pancreatic cancer is diagnosed -- from reacting to symptoms late in the disease to identifying patients at risk years earlier. "This temporal window holds profound significance, as attaining such early detection would substantially augment the probability of cure and improved survival," the researchers wrote. If confirmed in real-world screening, such tools could help move more cases into a window where surgery or other treatments are possible, which modeling studies suggest could significantly improve survival. "Modelling studies indicate that increasing the proportion of localized [pancreatic ductal carcinomas] from 10% to 50% would more than double survival rates, thereby underscoring that the timing of diagnosis is the single most critical determinant of survival outcomes," they said. The system, called Redmod, analyzes patterns in CT images that aren't visible to the human eye. It was trained and tested on scans from more than 1,400 people, including 219 patients whose earlier scans had been read as normal but who later developed pancreatic cancer. In a head-to-head comparison, the AI was markedly better than radiologists at picking up these early signs. It correctly identified 73% of cases, compared with about 39% for doctors reviewing the same images. The advantage widened for scans taken more than two years before diagnosis, where the system detected 68% of cases versus 23% for radiologists. The model also performed consistently across different hospitals and scanners, and correctly classified more than 80% of scans from people who didn't develop cancer. The tool could eventually be used to flag high-risk patients -- such as older adults with unexplained weight loss and new-onset diabetes -- for closer follow-up, the researchers said, but it needs prospective testing to confirm it improves outcomes before routine use.
[2]
AI model detects pancreatic cancer years before clinical diagnosis
BMJ GroupApr 28 2026 An AI model (REDMOD) can pick up the very early subtle tissue changes of pancreatic ductal adenocarcinoma, the most common form of pancreatic cancer, which conventional imaging and the human eye find difficult to detect, finds research published online in the journal Gut. As such, it offers the potential to shift an all too common late stage, terminal disease diagnosis to one that is at an early stage (stage 0) and treatable, say the researchers. While REDMOD was more accurate than experienced radiologists, it requires testing in high risk patients, defined as those with unexpected weight loss and newly diagnosed diabetes, before it can be widely used in clinical practice, they add. Pancreatic ductal adenocarcinoma has a poor rate of survival. It's usually diagnosed late, in the absence of symptoms and visible tissue changes in the early stages, and it rapidly progresses, explain the researchers. To overcome these challenges, the researchers developed an AI framework, called Radiomics-based Early Detection MODel (REDMOD), designed specifically to pick up the subtle tissue texture patterns (radiomics) of very early pancreatic cancer, which standard computed tomography (CT) scans can't see. The framework includes automated pancreatic segmentation-clear delineation of the borders of the pancreas from surrounding tissue/organs, obviating the need for this to be done manually with the attendant risk of variable accuracy. To test its reliability and effectiveness, the researchers applied REDMOD on abdominal CT scans from 219 patients from several different hospitals, who were deemed to show no evidence of disease after radiologist review, but who were subsequently diagnosed with pancreatic cancer. In 87 (40%), this was 3-12 months; in 76 (35%) this was 12-24 months; and in 56 (25%) more than 24 months (up to around 3 years) before diagnosis. Disease was located in the head of the pancreas in nearly two thirds (64%) of patients. Their scans were compared with those of a total of 1243 patients who hadn't developed the disease up to 3 years later, matched by age, sex, and scan date. The average age of those who were subsequently diagnosed with pancreatic cancer was 69, but ranged from 34 to 88; and the average age of the comparison group was 64, but ranged from 34 to 88. REDMOD detected the 'invisible' signature of pre-clinical pancreatic ductal adenocarcinoma an average of 475 days before clinical diagnosis. "This temporal window holds profound significance, as attaining such early detection would substantially augment the probability of cure and improved survival," highlight the researchers. "In fact, modelling studies indicate that increasing the proportion of localised [pancreatic ductal carcinomas] from 10% to 50% would more than double survival rates, thereby underscoring that the timing of diagnosis is the single most critical determinant of survival outcomes," they add. And REDMOD performed better than radiologists: it was nearly twice as sensitive-the ability to pick up true, rather than false, positive results-at accurately picking up 'invisible' early malignant cellular changes: 73% compared with 39%. And it was nearly 3 times as accurate as radiologists for cases detected more than 2 years before clinical diagnosis: 68% vs 23%. It also correctly identified just over 81% of scans in an independent group (539 patients) drawn from several hospitals and 87.5% in the public US National Institutes of Health NIH-PCT dataset (80 patients) as free of pancreatic cancer. The pre-clinical changes detected were a reliable indicator of subsequent clinical disease because REDMOD gave the same answer for 90-92% of scans when the same patient was scanned again some months earlier. The researchers acknowledge various limitations to their findings, including that they weren't based on an ethnically diverse group of patients. Nevertheless, they conclude: "This study validates REDMOD as a fully automated AI framework capable of identifying the imaging signatures of stage 0 [pancreatic ductal adenocarcinoma] in normal pancreas, achieving this with substantial lead times and performance superior to expert radiologists." They add: "While prospective validation is paramount to confirm clinical utility, the REDMOD framework represents a significant advance towards shifting the paradigm for sporadic [pancreatic ductal adenocarcinoma] from a late-stage symptomatic diagnosis to proactive pre-clinical interception, offering tangible hope for improving outcomes in this challenging disease." BMJ Group Journal reference: DOI: 10.1136/gutjnl-2025-337266
[3]
Mayo Clinic Says AI Can Detect Pancreatic Cancer Years Before Human Doctors - Decrypt
REDMOD's detection capability nearly doubles that of specialists reviewing the same scans -- 39% for radiologists versus 73% for the AI. Mayo Clinic has developed an AI model that can detect pancreatic cancer up to three years before clinical diagnosis by identifying subtle changes in routine CT scans, according to validation study results published in the journal, Gut. The AI model, called REDMOD, detected pancreatic cancer an average of 475 days before clinical diagnosis with 88% specificity. The system correctly identified patients who did not have the cancer while spotting what researchers described as an "invisible" signature of pre-clinical pancreatic ductal adenocarcinoma. "The greatest barrier to saving lives from pancreatic cancer has been our inability to see the disease when it is still curable," said Mayo Clinic Radiologist and Nuclear Medicine Specialist Ajit Goenka, M.D., the study's senior author.. "This AI can now identify the signature of cancer from a normal-appearing pancreas, and it can do so reliably over time and across diverse clinical settings." For cases detected more than two years before clinical diagnosis, REDMOD proved nearly three times as accurate as radiologists, achieving 68% accuracy compared to 23% for human specialists reviewing the same imaging. Mayo's breakthrough arrives amid broader AI advances in pancreatic cancer detection. PanDx, an AI framework for analyzing contrast-enhanced CT scans, recently achieved first place in the PANORAMA challenge with an AUROC of 0.9263. Mayo Clinic researchers are now conducting AI-PACED, a prospective clinical study evaluating how clinicians can integrate AI-guided detection into care for patients at elevated risk. The study aims to translate REDMOD's laboratory success into real-world clinical applications. Early detection remains crucial for pancreatic cancer, projected to become the second-leading cause of cancer-related death in the U.S. by 2030. The disease's lethality stems from its late presentation -- more than 85% of patients receive a diagnosis after the cancer has already spread, the same report noted.
[4]
AI finds signs of pancreatic cancer before tumors develop
The Mayo Clinic's AI model analyzes a CT scan to detect early tissue changes associated with pancreatic cancer.Mayo Clinic By the time doctors detect pancreatic cancer, it's often too late to treat effectively. But a new study suggests that artificial intelligence might be able to find signs of the disease before tumors are visible on a scan. An AI model developed at the Mayo Clinic in Rochester, Minnesota, detected abnormalities on patients' CT scans up to three years before they were diagnosed with pancreatic cancer, according to research published this week in the journal Gut. The scientists behind the model, which is now being evaluated in a clinical trial, trained it by feeding in CT scans from patients who had been screened for other medical conditions then were later diagnosed with pancreatic cancer. The team then had radiologists review the scans and compared their ability to find early signs of cancer to that of the AI model. The model was found to be three times better at identifying the early signs. "We knew, based on the biology of the disease, that this is not something which is coming all of a sudden in three months ... We knew that the signal was there. We just needed to find a way to be able to detect it," said Dr. Ajit Goenka, a radiologist at Mayo Clinic and an author of the study. With a five-year survival rate of 13%, pancreatic cancer is on track to become the second leading cause of cancer deaths by 2030. Around 80% of patients are diagnosed after the disease has reached an advanced stage. Unlike colon or breast cancer, there is no routine screening for pancreatic cancer in healthy people. Feeling for a lump is nearly impossible, since the pancreas is buried deep in the abdomen. And typical symptoms like stomach pain and sudden weight loss usually don't begin until the cancer has spread to other organs. Early markers of the disease are often too subtle to be seen by the human eye on a scan. In many cases, patients' scans appear normal as little as six months before they're diagnosed. "I analyze these images every day," said Dr. Daniel Jeong, a diagnostic radiologist at Moffitt Cancer Center who was not involved in the Mayo Clinic research. "We're really looking for a measurable mass that could represent the cancer. So these tumors need to grow to a certain level to become visible." Goenka said one signature of early cancer that the AI model was able to detect is abnormal cells in the pancreas that shelter and protect cancer from the body's immune defenses. Scientists have known such cells exist but struggled to find them on scans. Goenka said the model could someday be useful for people who already have risk factors for the disease -- such as a family history or diabetes -- but don't have any symptoms. From there, doctors would likely recommend additional blood work and imaging. "Unfortunately, if they have symptoms and if it's truly pancreas cancer, you don't need AI for that," he said. The AI model is one of several recent advancements in pancreatic cancer research. Last month, the results of an early-stage trial showed that an mRNA vaccine prolonged survival in eight patients with pancreatic cancer. An experimental drug called daraxonrasib was also found to double patients' life expectancy in a later-stage trial. The Food and Drug Administration said Friday that the drug's developer, Revolution Medicines, could expand access to it in a controlled setting for patients with advanced pancreatic cancer who have already tried other treatments. Daraxonrasib hasn't been FDA-approved yet. Additionally researchers are working on advanced blood tests that could look for hallmarks of the disease. "We're making, actually, major strides. It hasn't turned this disease around," said Dr. Tamas Gonda, director of the pancreatic disease program at NYU Langone's Perlmutter Cancer Center. Other doctors not affiliated with the Mayo Clinic study said that by catching signs of pancreatic cancer before it spreads to major organs or blood vessels, the AI model might increase the number of patients who could be candidates for surgery, chemotherapy or radiation. "This really could be a game changer for us for early detection," said Dr. Pam Hodul, a surgical oncologist at Moffitt Cancer Center. AI has shown increasing promise as a diagnostic tool for a range of other conditions. In a study published this week in the journal Science, researchers found that AI either matched or outperformed human physicians at diagnosing emergency room patients. Goenka said it could be a while before the Mayo Clinic's model reaches the public, since the clinical trial needs to follow participants for three to five years to see who develops cancer and who does not. "In a disease where we have been just wandering in darkness for decades, this is a milestone that shows us the finish line, but we still have to get to the finish line," he said.
[5]
Mayo Clinic AI Detects Pancreatic Cancer Up to 3 Years Before Diagnosis in Landmark Validation Study | Newswise
Newswise -- ROCHESTER, Minn. -- A Mayo Clinic-developed artificial intelligence (AI) model can help specialists detect pancreatic cancer on routine abdominal CT scans up to three years before clinical diagnosis. It identifies subtle signs of disease before tumors are visible, when curative treatment may still be possible. The findings, published in Gut, mark a milestone in Mayo Clinic's multiyear research effort to enable earlier detection of one of the deadliest cancers. The study validates this next-generation AI model using data and workflows that mirror clinical practice, including CT scans from multiple institutions, imaging systems and protocols. Researchers used the AI model to analyze nearly 2,000 CT scans, including scans from patients later diagnosed with pancreatic cancer -- all originally interpreted as normal. The system, called the Radiomics-based Early Detection Model (REDMOD), identified 73% of those prediagnostic cancers at a median of about 16 months before diagnosis -- nearly double the detection rate of specialists reviewing the same scans without AI assistance. The advantage was even greater at earlier time points. In scans obtained more than two years before diagnosis, the AI identified nearly three times as many early cancers that would otherwise go undetected. Pancreatic cancer remains one of the deadliest cancers because it rarely causes detectable signs in its earliest stages. More than 85% of patients receive a diagnosis after the disease has already spread, and five-year survival rates remain below 15%, according to the National Cancer Institute. Projections show it will become the second-leading cause of cancer-related death in the U.S. by 2030. "The greatest barrier to saving lives from pancreatic cancer has been our inability to see the disease when it is still curable," says Ajit Goenka, M.D., the study's senior author, and a Mayo Clinic radiologist and nuclear medicine specialist. "This AI can now identify the signature of cancer from a normal-appearing pancreas, and it can do so reliably over time and across diverse clinical settings." REDMOD measures hundreds of quantitative imaging features that describe tissue texture and structure, capturing faint biological changes as cancer begins to develop. The model is designed to analyze CT scans already obtained for other reasons -- particularly in high-risk patients, such as those with new-onset diabetes -- and flag elevated risk before any visible mass appears. The model runs automatically without time-intensive manual preparation. The team validated the model across CT scans from multiple institutions, imaging systems and protocols, demonstrating consistent performance beyond a single dataset. The model's predictions also remained stable over time. In patients with multiple scans, the AI produced consistent results months apart, supporting its use for longitudinal monitoring and early detection. Researchers are advancing this work into clinical testing through Artificial Intelligence for Pancreatic Cancer Early Detection, or AI-PACED. This prospective study evaluates how clinicians can integrate AI-guided detection into care for patients at elevated risk. The study combines AI analysis of routine imaging with longitudinal follow-up to assess performance, including early detection, false positives and clinical outcomes. This research is part of Mayo Clinic's Precure initiative, which aims to predict and prevent disease by identifying the earliest biological changes in the body before symptoms begin. It also reflects Mayo Clinic's Clinical Impact strategy, accelerating the translation of discovery into patient care. The study was supported by the National Institutes of Health, the Hoveida Family Foundation, the Mayo Clinic Comprehensive Cancer Center and the Champions for Hope Pancreas Cancer Research Program of the Funk-Zitiello Foundation. For a complete list of authors, disclosures and funding, review the study. ### About Mayo Clinic Mayo Clinic is a nonprofit organization committed to innovation in clinical practice, education and research, and providing compassion, expertise and answers to everyone who needs healing. Visit the Mayo Clinic News Network for additional Mayo Clinic news. About Mayo Clinic Comprehensive Cancer Center Designated as a comprehensive cancer center by the National Cancer Institute, Mayo Clinic Comprehensive Cancer Center is defining the cancer center of the future, focused on delivering the world's most exceptional patient-centered cancer care for everyone. At Mayo Clinic Comprehensive Cancer Center, a culture of innovation and collaboration is driving research breakthroughs in cancer detection, prevention and treatment to change lives.
[6]
Study shows AI outperforms radiologists in early detection
An artificial intelligence framework named REDMOD can identify the earliest signs of pancreatic cancer on routine CT scans an average of 475 days before typical clinical diagnosis, according to a study published in the journal Gut. Developed by researchers at Mayo Clinic, REDMOD detects subtle tissue texture changes associated with pancreatic ductal adenocarcinoma that are not visible to the human eye or traditional imaging techniques. REDMOD exhibits nearly twice the sensitivity of experienced radiologists, achieving an accuracy rate of 73% in detecting preclinical disease, compared to 39% for radiologists. For cases identified more than two years before clinical diagnosis, REDMOD's accuracy soars to 68%, while radiologists' accuracy drops to 23%. The model also classified over 81% of scans as cancer-free in an independent cohort of 539 patients and recorded an accuracy of 87.5% in the NIH-PCT dataset of 80 patients. Additionally, REDMOD demonstrated consistent results upon retesting the same patients months later, achieving consistency rates of 90 to 92%. Pancreatic cancer remains a critical health issue, being the deadliest major cancer in the United States with a five-year survival rate of just 13%. It is the third-leading cause of cancer-related deaths, with an estimated 67,530 new diagnoses and 52,740 deaths expected in 2023. If detected at a localized stage, the five-year survival rate increases significantly to 44%. The researchers emphasize that REDMOD's ability to detect cancer early could greatly enhance the probability of cure and improve survival outcomes. "This temporal window holds profound significance, as attaining such early detection would substantially augment the probability of cure and improved survival," the researchers stated. REDMOD utilizes automated pancreatic segmentation, reducing the reliance on radiologists to manually outline pancreatic borders, a process that is often time-consuming. However, the team noted that prospective validation in high-risk patients is necessary before REDMOD can be broadly implemented in clinical practice. They referred to this tool as a significant advance in shifting pancreatic cancer diagnosis from late-stage symptomatic detection to early pre-clinical interception.
[7]
How AI Is Spotting Pancreatic Cancer Signals That Most Doctors Miss
Artificial intelligence may be able to detect pancreatic cancer more than a year before it's typically diagnosed, offering a potential breakthrough for one of the deadliest forms of cancer. Researchers at the Mayo Clinic developed a model called Redmond that identified subtle warning signs in routine CT scans an average of about 475 days before patients were diagnosed, according to a study published Tuesday in the journal Gut. The system works by analyzing patterns in imaging that are invisible to the human eye. It was trained and tested on more than 1,400 patients, including 219 people whose scans were initially read as normal but who later developed pancreatic cancer, Bloomberg reported. In head-to-head comparisons, the AI significantly outperformed radiologists at spotting these early signals. It correctly identified 73 percent of cases, compared with about 39 percent for doctors reviewing the same images. The gap widened further for scans taken more than two years before diagnosis, where the model detected 68 percent of cases versus 23 percent for radiologists, according to Bloomberg.
[8]
Cancer Never Saw the Algorithm Coming | PYMNTS.com
By completing this form, you agree to receive marketing communications from PYMNTS and to the sharing of your information with our sponsor, if applicable, in accordance with our Privacy Policy and Terms and Conditions. The same week that a new philanthropic push pledged $500 million to build artificial intelligence (AI) systems that model disease at the cellular level, two separate research teams published evidence that AI can already see what radiologists cannot. The numbers behind Mayo Clinic's new AI are striking. A Mayo Clinic-developed model called REDMOD can detect pancreatic cancer on routine abdominal CT scans up to three years before a clinical diagnosis, identifying subtle signs of disease before tumors are visible, when curative treatment may still be possible, Mayo Clinic News Network reported Wednesday (April 29). Researchers analyzed nearly 2,000 CT scans, including scans from patients later diagnosed with pancreatic cancer that were originally interpreted as normal. REDMOD identified 73% of those prediagnostic cancers at a median of about 16 months before diagnosis, nearly double the detection rate of specialists reviewing the same scans without AI assistance. The advantage compounded over time. In scans obtained more than two years before diagnosis, the AI identified nearly three times as many early cancers that would otherwise go undetected, Mayo Clinic News Network reported. The stakes are real. More than 85% of pancreatic cancer patients receive a diagnosis after the disease has already spread, and five-year survival rates remain below 15%, according to the National Cancer Institute. Projections show pancreatic cancer will become the second-leading cause of cancer-related death in the U.S. by 2030. REDMOD works by measuring quantitative imaging features that describe tissue texture and structure, capturing faint biological changes before any visible mass forms. The model runs automatically without time-intensive manual preparation and was validated across CT scans from multiple institutions, imaging systems and protocols, Mayo Clinic News Network reported. It is designed to analyze scans already obtained for other reasons, particularly in high-risk patients such as those with new-onset diabetes. The same week, Alibaba's research arm Damo Academy published results for a parallel effort targeting colorectal cancer. Its Coca AI model accurately identified five previously missed cases of colorectal cancer from the non-contrast CT scans of more than 27,000 people, achieving a sensitivity of 86.6% and a specificity of 99.8%. Damo Academy said Coca outperformed 10 radiologists of varying experience levels by 20.4% on sensitivity, the South China Morning Post reported. The research was developed with Chinese institutions including Guangdong General Hospital and published in the Annals of Oncology. Current diagnostic methods for colorectal cancer, including colonoscopy and CT colonography, are invasive and create discomfort for patients, whereas Coca has the potential to be a non-invasive, cost-effective and scalable tool, according to Damo researchers. The detection breakthroughs matter. But the infrastructure bet announced the same week signals where the field is heading. The Chan Zuckerberg Biohub committed $500 million over five years to AI-driven biology, with $400 million going toward its own work and $100 million aimed at spurring others, Axios reported Wednesday. According to the report, Zuckerberg said last year that Biohub's long-term goal is to cure all human disease through the intersection of AI and biology. The stated goal is not incremental. Biohub chief Alex Rives told Axios that the usefulness of an AI model's prediction increases exponentially as the scale of the data grows. Most current datasets cover about a billion cells. The aim is to reach an order of magnitude or more beyond that, Rives said. Biohub is focused on frontier AI and frontier biology, using large-scale models for virtual cells, immune reprogramming and disease prediction, Fortune reported. The ambition sits upstream of what REDMOD and Coca are doing. Scan-reading AI catches disease once the body has already started changing. A virtual cell model, if it works as theorized, could predict which patients will reach that point at all.
[9]
New tool can find deadliest cancer years before tumors can be seen on a scan
Many are split on whether AI is good for humanity, but a new AI-powered tool could prove revolutionary when it comes to cancer screenings. Pancreatic cancer is considered one of the most aggressive and difficult-to-detect cancers. It has a 13% five-year survival rate and is projected to cause more than 52,700 deaths this year, according to the American Cancer Society. An AI model developed at the Mayo Clinic could be the answer to improving those numbers since it detected abnormalities on CT scans up to three years before a pancreatic cancer diagnosis. The research, published this week in the journal Gut, evaluated scans of patients who had been screened for other conditions and later diagnosed with pancreatic cancer. Radiologists and the AI model were tasked with reviewing the scans and finding early signs of cancer. The outcome? The robot was three times better at identifying early signs that aren't detectable by the human eye. "Early symptoms, such as back pain, fatigue, weight loss or digestive discomfort, are vague and often mistaken for other, less serious conditions," Dr. Diane Simeone, director of Moores Cancer Center at UC San Diego Health, previously told The Post. Pancreatic cancer develops from abnormal cell growth within the pancreas, a vital organ that plays a crucial role in digestion and blood sugar regulation. One thing the model was able to detect that scientists and doctors have previously struggled to find was abnormal pancreatic cells that protect the disease from immune defenses. "We knew, based on the biology of the disease, that this is not something which is coming all of a sudden in three months," Dr. Ajit Goenka, a radiologist at the Mayo Clinic and an author of the study, told NBC. "We knew that the signal was there. We just needed to find a way to be able to detect it," he added. Goenka's team hopes the new medical tool, which is in clinical trials, will help those with a family history who aren't experiencing symptoms. There's no long-term cure for pancreatic cancer, but treatment strategies like surgery, chemotherapy, targeted therapies and immunotherapy can help manage the disease. In other AI news, a study published in the New England Journal of Medicine found that people prefer medical advice from AI bots over a doctor or online healthcare platforms, despite the information often being wrong. Some AI experts warn that these tools cannot substitute for the judgment, ethical accountability or lived experience of medical professionals. "Keeping humans in the loop isn't optional -- it's the safeguard that protects lives," Andy Kurtzig, CEO of the AI-powered search engine Pearl.com, previously told The Post.
Share
Copy Link
Mayo Clinic researchers developed REDMOD, an AI model that spots pancreatic cancer an average of 475 days before clinical diagnosis by identifying subtle changes invisible to the human eye on routine CT scans. The system correctly identified 73% of cases compared to 39% for radiologists, offering hope for shifting diagnosis from late-stage terminal disease to early-stage curative treatment.
AI Model REDMOD Achieves Breakthrough in Early Detection
Mayo Clinic researchers have developed an AI system that can detect pancreatic cancer on routine CT scans up to three years before clinical diagnosis, according to a validation study published in the journal Gut
1
. The AI model, called Radiomics-based Early Detection Model (REDMOD), identified the invisible signature of pre-clinical pancreatic ductal adenocarcinoma an average of 475 days before patients received their diagnosis2
. This temporal window holds profound significance for a disease where more than 85% of cases are found at a stage where curative treatment is no longer possible1
.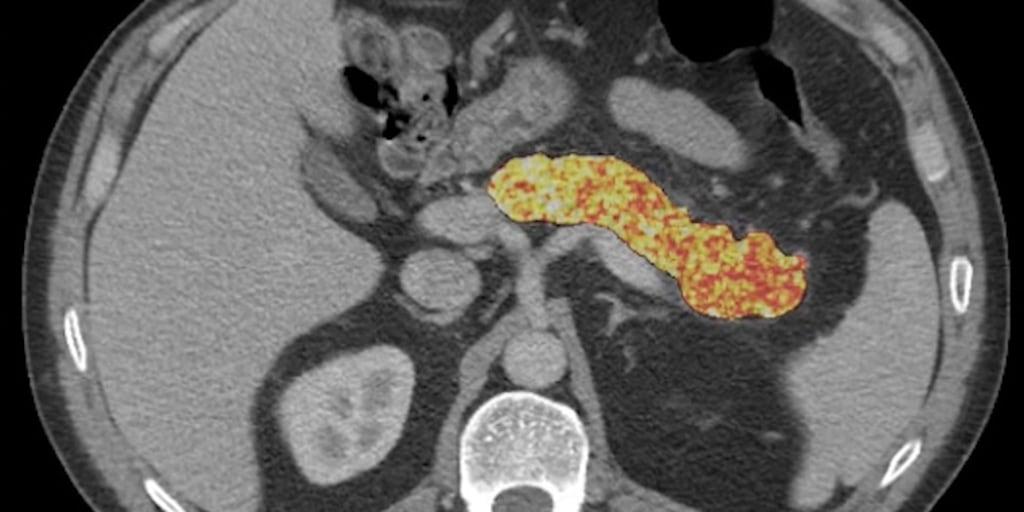
Source: NBC
The system analyzes patterns and tissue texture in imaging that aren't visible to the human eye, identifying subtle changes that signal cancer development before tumors appear
4
. REDMOD includes automated pancreatic segmentation, which clearly delineates the borders of the pancreas from surrounding tissue and organs, eliminating the need for manual preparation and reducing the risk of variable accuracy2
.
Source: PYMNTS
AI Outperforms Radiologists in Identifying Early Indicators of Pancreatic Cancer
In head-to-head testing, REDMOD demonstrated markedly superior performance compared to experienced radiologists reviewing the same CT scans. The AI correctly identified 73% of prediagnostic cancers, nearly double the 39% detection rate achieved by specialists analyzing identical images without AI assistance
5
. The advantage widened dramatically for scans obtained more than two years before diagnosis, where the system detected 68% of cases versus just 23% for radiologists1
.Researchers tested the AI framework on abdominal CT scans from 219 patients across several hospitals who showed no evidence of disease after radiologist review but were subsequently diagnosed with pancreatic cancer
2
. These scans were compared with those from 1,243 patients who hadn't developed the disease up to three years later. The model also correctly identified more than 81% of scans from people who didn't develop cancer, demonstrating strong specificity alongside its sensitivity1
.Detects Cancer Years Before Diagnosis Could Transform Survival Rates
"The greatest barrier to saving lives from pancreatic cancer has been our inability to see the disease when it is still curable," said Dr. Ajit Goenka, a Mayo Clinic radiologist and the study's senior author
3
. The timing of diagnosis represents the single most critical determinant of survival outcomes for this deadly disease. Modeling studies indicate that increasing the proportion of localized pancreatic ductal carcinomas from 10% to 50% would more than double survival rates1
.
Source: Decrypt
Pancreatic cancer remains one of the deadliest malignancies, with five-year survival rates hovering around 10% globally
1
. The disease is projected to become the second-leading cause of cancer-related death in the United States by 20303
. It's rarely detected early because tumors typically don't cause symptoms and often aren't visible on medical diagnostics until the disease has advanced. Early markers are too subtle to be seen by the human eye on a scan, and in many cases, patients' scans appear normal as little as six months before diagnosis4
.Related Stories
Identifying Subtle Changes in CT Scans Across Multiple Clinical Settings
REDMOD performed consistently across different hospitals, imaging systems, and scanning protocols, demonstrating its robustness beyond a single dataset
5
. The model's predictions remained stable over time, producing consistent results when the same patient was scanned months apart, with REDMOD giving the same answer for 90-92% of scans2
. This reliability supports its potential use for longitudinal monitoring and early detection in high-risk patients.One signature the AI identifies is abnormal cells in the pancreas that shelter and protect cancer from the body's immune defenses—cells that scientists have known exist but struggled to find on scans
4
. The system measures hundreds of quantitative imaging features that describe tissue texture and structure, capturing faint biological changes as cancer begins to develop5
.Path to Clinical Implementation and Improving Survival Rates
The tool could eventually be used to flag high-risk patients for closer follow-up, particularly older adults with unexplained weight loss and new-onset diabetes
1
. Mayo Clinic is now conducting AI-PACED, a prospective clinical trial evaluating how clinicians can integrate AI-guided detection into care for patients at elevated risk3
. The study combines AI analysis of routine imaging with longitudinal follow-up to assess performance, including early detection rates, false positives, and clinical outcomes5
.By catching signs before cancer spreads to major organs or blood vessels, the system might increase the number of patients who could be candidates for surgery, chemotherapy, or radiation
4
. However, the model needs prospective testing to confirm it improves outcomes before routine use1
. Goenka noted it could be several years before the technology reaches widespread clinical use, as clinical trials need to follow participants for three to five years to validate real-world effectiveness4
.References
Summarized by
Navi
Related Stories
AI model detects hidden pancreatic cancer up to 3 years before doctors spot it on CT scans
07 May 2026•Health
AI Revolutionizes Breast Cancer Detection: New Tools Predict Risk and Catch Missed Tumors
22 Oct 2025•Health

AI Breakthrough: Deep Learning Model Revolutionizes Pancreatic Cancer Diagnosis and Treatment
13 Dec 2024•Health








